Male Reproductive System: Sertoli Cells
Can you identify the seminiferous tubules in the picture?
Spermatogenesis takes place in
the seminiferous tubules. This includes mitosis
and meosis to form haploid gametes, followed by maturation to form
spermatocytes (called spermiogenesis). The stages that a developing
spermatogonium passes through as it develops and matures to form
a mature spermatozoon are covered in more detail here.
The seminiferous tubules are lined by a complex
stratified epithelium containing two distinct populations of cells,
spermatogenic cells, that develop into spermatozoa,
and Sertoli cells which have a supportive and nutrient
function.
Can you identify Sertoli cells, and cells in
different stages of spermatogenesis and spermiogenesis in this image?
(Use the diagram below to help you).
Where do you expect to find type A spermatogonia, primary and secondary
spermatocytes, spermatids and mature spermatozoa. Between which stages does meiosis occur?
Sertoli cells are the epithelial supporting cells of the seminiferous tubules. They are derived from the epithelial
sex cords of the developing gonads. They are tall simple columnar cells, which span from the basement membrane to the lumen. They
surround the proliferating and differentiating germ cells forming pockets around these cells, providing nutrients, and phagocytosing excess spermatid cytoplasm, not needed in forming the spermatozoa.
They are connected to each other by continuous tight junctions that seal the tubule into two compartments: the basal (close to
the basal lamina) and adluminal (towards the lumen) compartment. Large molecules cannot pass between the basal and adluminal compartment
- this is called the blood-testis barrier.
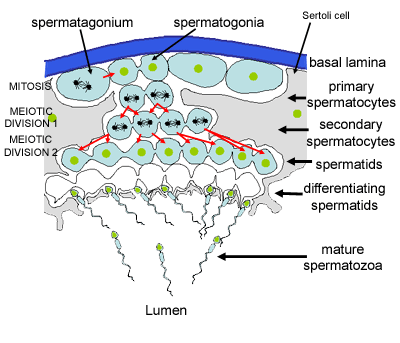
This is a schematic diagram of part of a seminiferous tubule, showing the stages in the formation of spermatozoa.
Like all epithelial cells, the Sertoli
cells are avascular. Sertoli cells
suport the germ cell progenitors and help to transfer nutrients
from the nearby capillaries. The developing spermatogonia rely on
the Sertoli cells for all of their nourishment. The blood-testis
barrier formed by the Sertoli cells effectively isolates
the developing spermatogonia, spermatocytes, spermatids and mature
spermatozoa from blood. Differentiating spermatozoa nestle in pockets
in the peripheral cytoplasm of these cells.
Sertoli cells also produce testicular
fluid, including a protein that binds to and concentrates
testosterone, which is essential for the development
of the spermatozoa. They also help to translocate the differentiating
cells to the lumen, and phagocytose degenerating germ cells and
surplus cytoplasm remaining from spermiogenesis.
Blood-testis barrier: Importantly, the basal regions
of the lateral borders of the Sertoli cells are
connected to each other by continuous tight junctions.
These divide the tubules into two separate compartments. The mitotic
spermatogonia remain in the basal compartment.
Differentiating progeny enter the adluminal compartment,
and are sealed off from the basal compartment. If novel antigens
are expressed on the haploid cells, then it is less likely that
they will be detected by the immune system in this sealed off compartment.
The developing cells are also in a very protective environment.
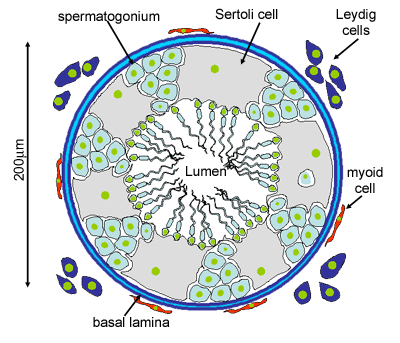
This diagram shows a single seminiferous tubule,
and cells in the interstitial tissue outside the tubule. In thisconnective
tissue between the seminiferous tubules there are large cells with
eosinophilllic cytoplasm called Leydig cells.
There are also cells called myoid cells surrounding
the basement membrane, which are squamous contractile cells, and
generate peristaltic waves in the tubules.
This image shows Leydig cells. Can you identify Leydig cells in the image shown here?
Leydig cells are 'interstitial' cells (as they lie between the tubules). They have pale cytoplasm because they
contain many cholesterol-lipid droplets. The Leydig cells make and secrete testosterone, in response
to lutenising hormone from the pituitary. The cholesterol is used in the first step of testosterone production.
Testosterone promotes production of spermatozoa, secretion from the accessory sex glands, and acquisition of male
secondary characteristics. This process does not start until puberty when LH stimulates the Leydig cells to produce testosterone.
FSH stimulates the Sertoli cells to secrete androgen-binding protein into the lumen of the seminiferous tubules. Binding of testosterone
in the lumen provides a local testosterone supply for the developing permatogonia.

